Introduction
Following the recommendations set out in the Rethinking Schizophrenia Care Pathway in Europe study paper, the next phase of the project — Country Profiles: Beyond Mental Health – A Brain Health Approach to Schizophrenia Prevention and Care — focuses on analysing country-specific models of care and identifying opportunities to improve prevention, early detection and integrated care across Europe. After a roundtable meeting in Poland in June 2025 and a webinar exploring the Danish context in December 2025, the project continued with a dedicated Germany-focused webinar on 4 March 2026. The event was organised by the European Brain Council (EBC) and the German Brain Council, together with the Department of Psychiatry and Psychotherapy of the University of Munich and the Department of Psychiatry and Psychotherapy of the University of Lübeck. The webinar, titled "AI-supported prediction and intervention: A comprehensive approach to integrated biopsychosocial schizophrenia care", brought together clinicians, researchers, policymakers, patient advocates and representatives from mental health organisations to discuss current developments and challenges in schizophrenia prevention and care in Germany. The programme featured presentations covering AI-supported early detection, translational research linking genetics to brain function, innovative care delivery models such as inpatient-equivalent home treatment, lifestyle interventions, and the perspective of families and caregivers. These contributions were followed by a roundtable discussion on future directions for improving schizophrenia care within a broader European brain health framework.
Opening address by Prof. Peter Falkai
In his opening remarks, Prof. Peter Falkai (Department of Psychiatry and Psychotherapy, University of Munich) welcomed participants and emphasised the importance of advancing schizophrenia care through a comprehensive brain health approach that integrates prevention, early detection and long-term recovery support. He highlighted that schizophrenia remains one of the most complex psychiatric disorders, often emerging in adolescence or early adulthood and requiring coordinated action across healthcare, social and community services.
Prof. Falkai also stressed the importance of combining scientific innovation with system-level transformation, noting that advances in digital technologies, neuroscience and personalised medicine offer new opportunities to improve early identification and treatment outcomes. He underlined that initiatives such as the Rethinking Schizophrenia project provide a valuable platform to translate scientific progress into improved care pathways and policy development across Europe.
“Schizophrenia care must move beyond a purely psychiatric perspective and embrace a broader brain health approach that integrates prevention, early detection and long-term recovery.”
The Rethinking Schizophrenia Project – European perspective by Prof. Pavel Mohr
Prof. Mohr (National Institute of Mental Health, Prague) introduced the Rethinking Schizophrenia project, which evaluates schizophrenia care models across nine European countries. The initiative aims to identify systemic gaps, assess outcomes and propose strategies to strengthen integrated care pathways across Europe.
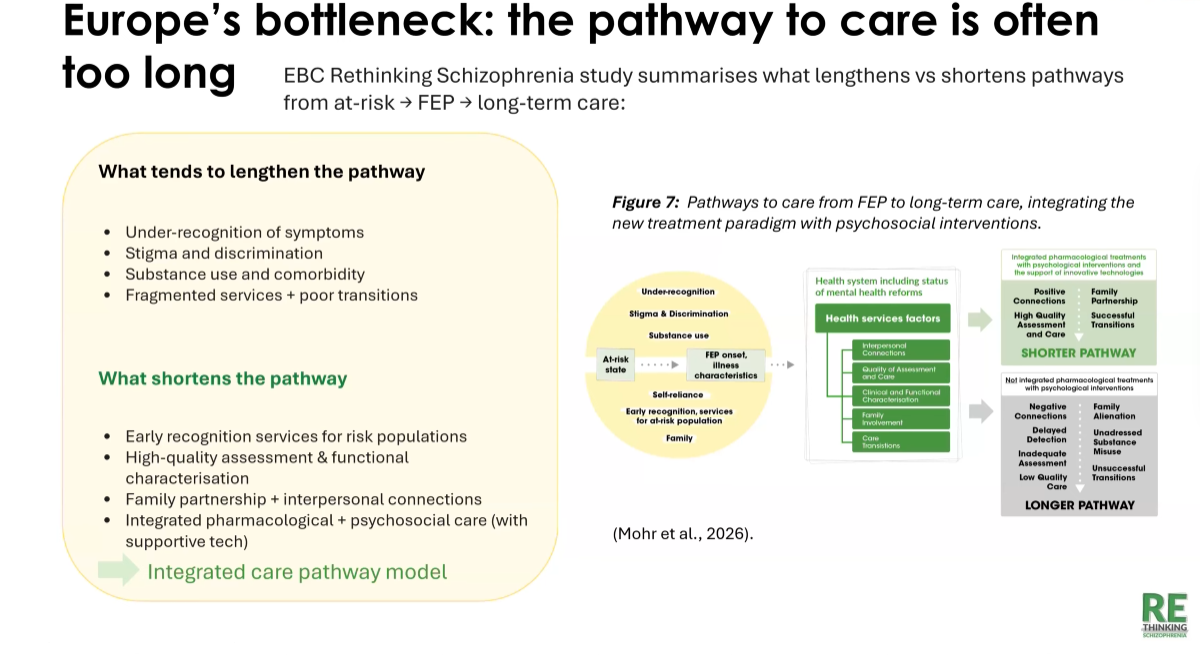
The study involved a survey of more than 200 mental health professionals, assessing access to services, care continuity and recovery outcomes. The findings highlight significant challenges across Europe. More than half of respondents considered national schizophrenia care systems inadequate, while many reported limited access to community mental health services. Early detection services were available in less than half of the cases reported. The study also highlighted barriers affecting recovery and long-term care, including lack of social support, negative symptoms and cognitive impairment. Fragmented services and delayed recognition of symptoms were identified as factors that prolong pathways to care.
The project proposes eight strategic action areas, including strengthening early detection programmes, expanding psychosocial interventions, improving workforce capacity and investing in research and data-driven decision-making.
“Across Europe we see important gaps in early detection, continuity of care and community services. Addressing these systemic issues is essential to improving outcomes for people living with schizophrenia.”
AI-supported early detection and intervention by Prof. Nikolaos Koutsouleris and Dr. Léon Franzen
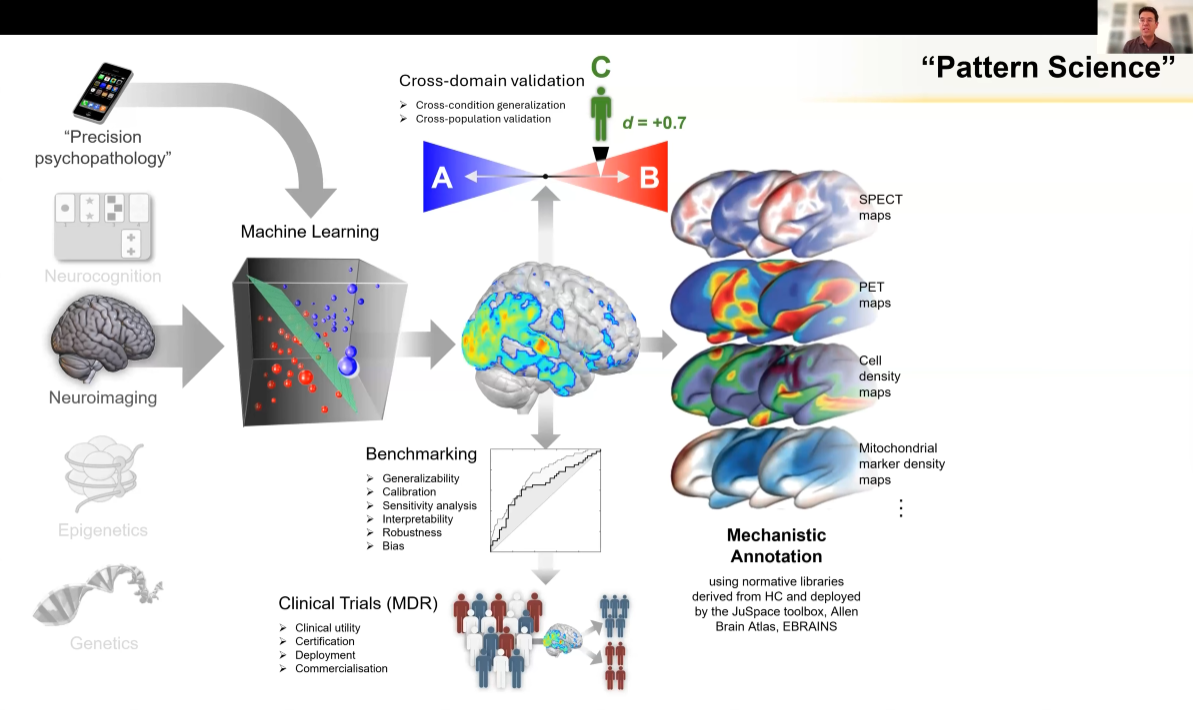
Prof. Nikolaos Koutsouleris (Ludwig-Maximilians University Munich) presented advances in machine learning and artificial intelligence for early detection of psychosis. His research focuses on integrating large multimodal datasets, including clinical information, neuroimaging, genetic data and cognitive assessments, to improve the prediction of psychosis risk. AI-based models can identify patterns that are not detectable through traditional clinical assessment alone, enabling clinicians to stratify individuals according to risk levels and personalise preventive interventions. This approach has the potential to support earlier diagnosis and reduce the transition from high-risk states to full psychotic disorders.
Prof. Koutsouleris emphasised that while these technologies show significant promise, their successful implementation requires robust validation, ethical oversight and careful integration into clinical decision-making processes.
Dr Léon Franzen (University of Lübeck) presented the PASTA project (Preterm-to-Adolescent Specifically Tailored Assessment), which aims to identify risk markers for psychiatric disorders during adolescence. By analysing clinical, biological and behavioural data, AI tools can support clinicians in detecting patterns that indicate increased risk of psychosis much earlier.
Such approaches have the potential to improve risk stratification and enable preventive interventions earlier in the disease trajectory. Early identification of individuals at high risk could reduce the likelihood of progression to full psychosis and improve long-term functional outcomes.
However, both speakers emphasised that predictive models must be carefully validated and integrated into clinical workflows in ways that support clinicians and protect patient rights.
“Artificial intelligence can help us detect psychosis risk earlier and support personalised interventions, but it must always complement clinical expertise and be implemented responsibly.”
“Early identification of risk during adolescence opens an important window of opportunity for prevention and early intervention in severe mental disorders.”
From genetics to animal models: understanding disease mechanisms by Prof. Sabine Hölter-Koch
Prof. Hölter-Koch (Helmholtz Munich) presented research exploring how genetic findings can be translated into insights about brain function and psychiatric disease mechanisms.
Schizophrenia is a highly complex disorder with both common genetic variants and rare mutations contributing to risk. Recent genomic studies have identified hundreds of associated loci but understanding how these genetic factors influence brain function remains a major scientific challenge. In genetics, an associated locus (plural: loci) refers to a specific location on a chromosome that has been statistically linked to a disease or trait through genetic studies. In schizophrenia research, large genome-wide association studies (GWAS) have identified hundreds of loci associated with increased risk of the disorder. These loci do not represent single “schizophrenia genes”; rather, they indicate regions of the genome where genetic variations contribute to disease susceptibility. Many of these loci influence biological processes such as synaptic signalling, neuronal development and neurotransmitter systems, helping researchers understand the complex biological mechanisms underlying schizophrenia.
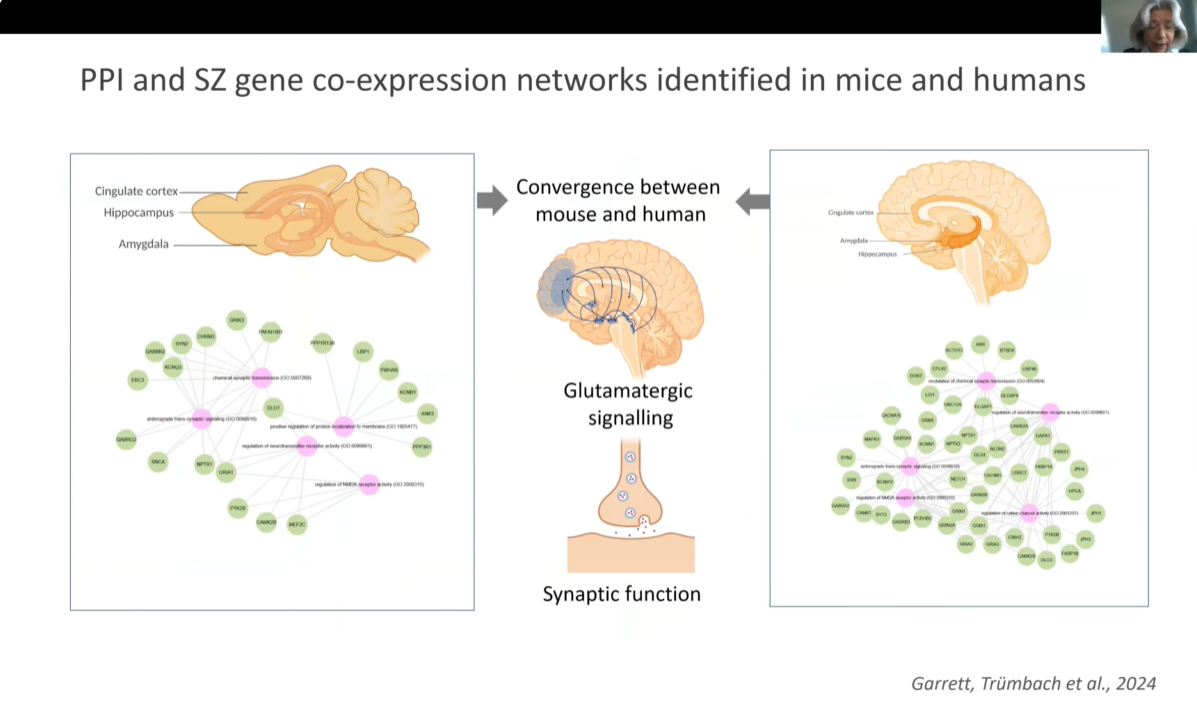
By combining genomic data with brain transcriptome mapping and animal models, researchers can better understand how disease-related genes affect neural circuits. Mouse models and behavioural phenotypes such as prepulse inhibition (PPI) provide valuable tools to study mechanisms relevant to schizophrenia.
These approaches enable researchers to identify candidate genes and pathways involved in synaptic function and glutamatergic signalling, helping to bridge the gap between genetic discoveries and clinical applications.
“Understanding how genetic variation affects brain function is key to unlocking the biological mechanisms underlying schizophrenia.”
Inpatient-equivalent psychiatric care (StäB) by Prof. Andreas Bechdolf
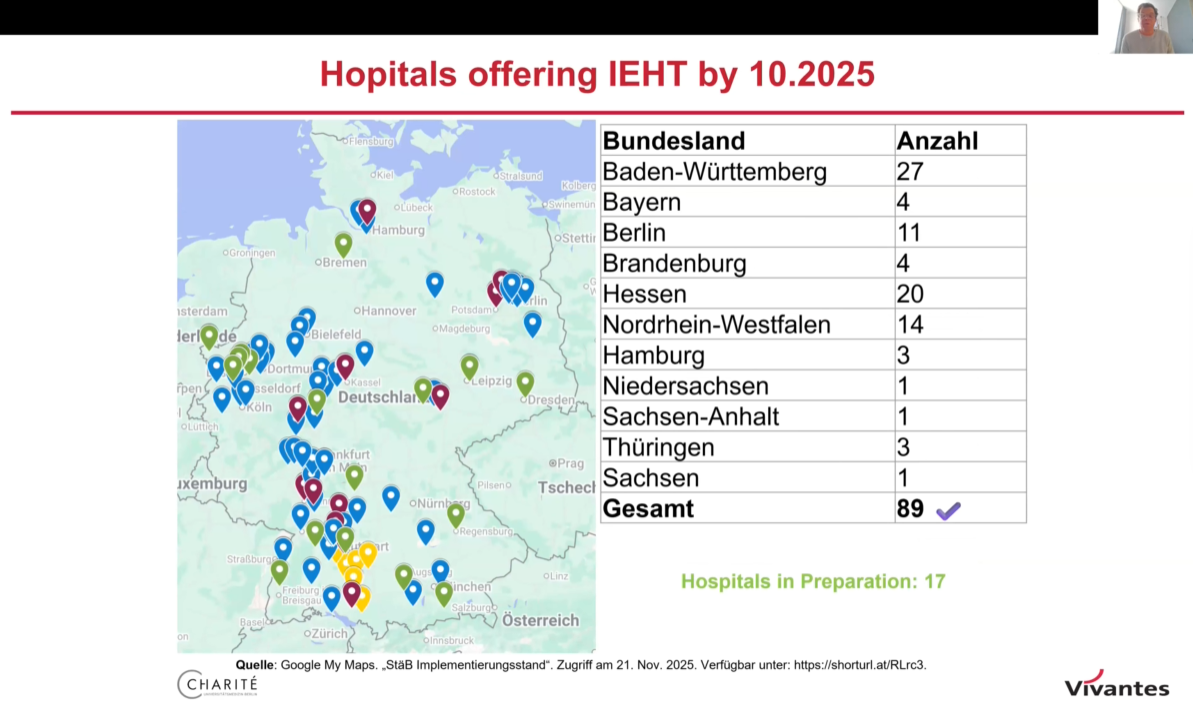
Prof. Bechdolf (Charité/Vivantes Berlin) presented evidence on inpatient-equivalent home treatment (StäB), a model introduced in Germany through legislation in 2018.
This approach allows hospital-based multidisciplinary teams to deliver intensive psychiatric treatment directly in a patient’s home environment. Daily visits and structured treatment protocols ensure that patients receive care equivalent to inpatient services while remaining in their familiar surroundings.
Evidence from a multicentre cohort study comparing home treatment with traditional inpatient care found similar clinical outcomes across several indicators, including symptom severity, quality of life and employment integration.
However, the home treatment model demonstrated higher patient satisfaction, greater involvement in decision-making and reduced reliance on hospital services over time. The model is increasingly implemented in Germany and represents an important step towards more recovery-oriented mental health care.
“Home-based treatment models can provide hospital-level care while improving patient satisfaction and participation in treatment decisions.”
Lifestyle and exercise interventions by Prof. Rebekka Lencer
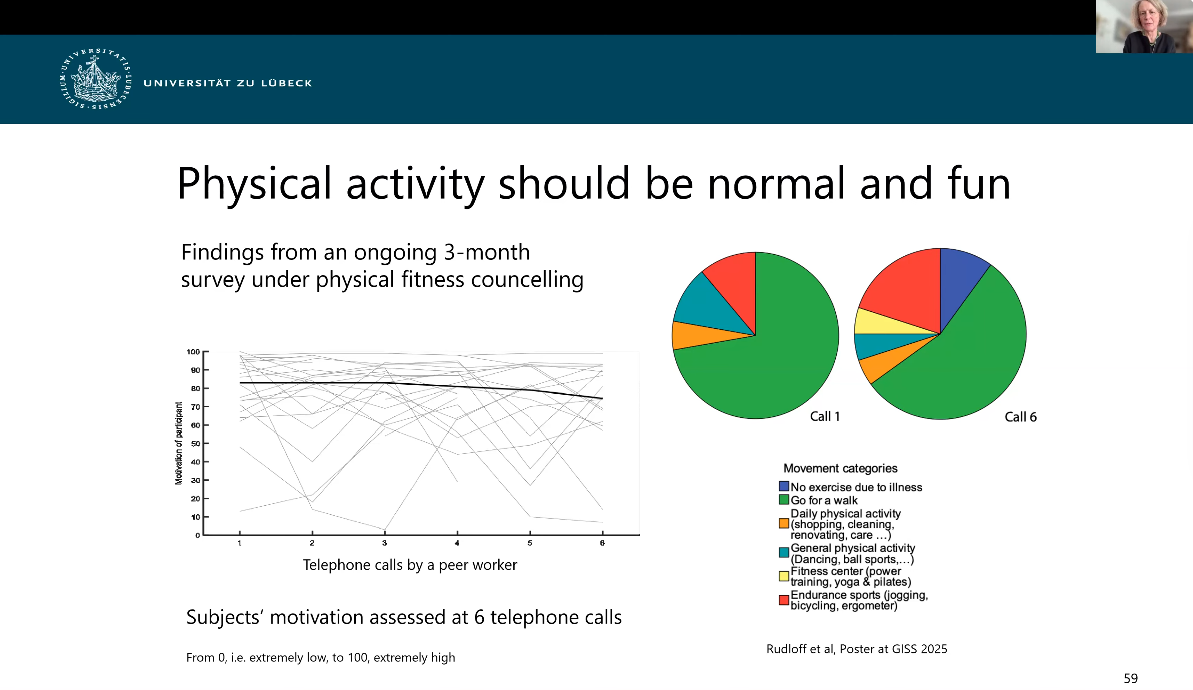
Prof. Lencer (University of Münster/University of Lübeck) highlighted the role of lifestyle interventions in schizophrenia treatment, particularly the benefits of physical activity.
Medication remains an essential component of treatment, but pharmacological approaches alone are often insufficient. Many patients experience metabolic side effects from antipsychotic medication, and treatment adherence can be challenging.
Exercise and lifestyle interventions can help to improve metabolic health, cognitive functioning and overall wellbeing. Physical activity has also been associated with structural changes in the brain, including improvements in hippocampal volume.
However, barriers such as low motivation, negative symptoms and self-stigma can limit participation. To overcome these challenges, programmes should focus on individualised fitness plans, motivational support and peer engagement.
“Lifestyle interventions and physical activity should be seen as essential components of schizophrenia care, supporting both mental and physical health.”
Perspective of families and caregivers by Gabriele Glocker
The webinar also included an important perspective from families and caregivers.
Gabriele Glocker (Federal Association of Relatives of Mentally Ill People (BApK)) highlighted several major challenges faced by families supporting individuals with schizophrenia in Germany. These include persistent stigma, fragmented welfare systems, and shortages of mental health professionals.
Families often experience significant stress when patients refuse treatment due to lack of insight into their condition. In addition, gaps in coordination between hospital services and community care can make it difficult to ensure continuity of support after discharge.
The presentation emphasised the need for greater involvement of families in care planning, stronger support structures for caregivers and reductions in stigmatization from clinicians.
“The country profiles in Poland, Denmark and Germany provide a strong evidence base to advance integrated care pathways for schizophrenia, which will be further consolidated in our upcoming European Psychiatry publication.”
Roundtable Discussion
The webinar concluded with a roundtable discussion moderated by Prof. Peter Falkai (University of Munich, European Brain Council), bringing together perspectives from clinical research, policy and patient advocacy. Participants included Prof. Andreas Meyer-Lindenberg (German Brain Council), Prof. Christoph Correll (Charité University Medicine Berlin), Bernhard Seidenath (Member of the Bavarian State Parliament), and Gabrielle Glocker (Federal Association of Relatives of Mentally Ill People – BApK).
Prof. Andreas Meyer-Lindenberg highlighted the importance of linking advances in neuroscience and genetics with improvements in clinical care pathways. He emphasised that schizophrenia should be increasingly addressed within a broader brain health framework, where early identification, prevention and long-term functional recovery are central objectives. Strengthening collaboration between research institutions and health systems was identified as a key priority to ensure that scientific discoveries translate into real improvements for patients.
Prof. Christoph Correll stressed the importance of early intervention and integrated treatment approaches, particularly during the early stages of psychosis. He noted that combining pharmacological treatment with psychosocial interventions, lifestyle approaches and digital tools can significantly improve long-term outcomes. Prof. Correll also highlighted the potential of data-driven and personalised medicine approaches, including AI-supported risk prediction, to support more targeted and preventive care strategies.
From a policy perspective, Bernhard Seidenath, Member of the Bavarian State Parliament, underlined the need to strengthen mental health services and ensure sustainable investment in prevention, treatment and rehabilitation. He emphasised that innovative care models—such as community-based services and home treatment approaches—should be further supported to improve accessibility and continuity of care. Mr. Seidenath also stressed the importance of reducing stigma and improving public awareness of schizophrenia. He pointed out that some German states have good care in place that other states could benefit from adopting. Representing the perspective of families and caregivers, Gabrielle Glocker reiterated the challenges faced by relatives supporting individuals living with schizophrenia. She highlighted the need for greater involvement of families in care planning, improved coordination between hospital and community services, and stronger support structures for caregivers. Addressing stigma and improving access to information and support were identified as key priorities for improving outcomes and quality of life for patients and their families.
Overall, the roundtable discussion emphasised the need for greater integration across research, clinical practice, policy and lived experience. Participants agreed that strengthening early detection, improving continuity of care and promoting recovery-oriented services are essential steps toward a more comprehensive and effective approach to schizophrenia prevention and care in Germany and across Europe.
The discussion reinforced the value of approaching schizophrenia within a broader brain health framework, which recognises the interconnected nature of neurological and psychiatric disorders and promotes prevention across the lifespan.
“Early, integrated and personalised treatment approaches offer the best chance to improve long-term outcomes for people with schizophrenia.”
“Early, integrated and personalised treatment approaches offer the best chance to improve long-term outcomes for people with schizophrenia.”
“Reducing stigma and strengthening mental health services are essential policy priorities to ensure better support for patients and families.”
“Families often carry a heavy burden. Greater involvement of relatives and better coordination of services are crucial to improving care.”
Conclusion and Next Steps
Prof. Peter Falkai and Frédéric Destrebecq (Executive Director, European Brain Council) closed the meeting. The Germany webinar represents an important milestone in the Country Profiles phase of the Rethinking Schizophrenia project. By bringing together diverse perspectives from research, clinical practice, policy and lived experience, the event provided valuable insights into the strengths and challenges of schizophrenia care in Germany.
Key themes emerging from the discussions include the importance of early detection, integrated biopsychosocial care, innovative service models and stronger support for families and caregivers.
The insights generated through the Germany webinar will contribute to the broader European analysis of schizophrenia care pathways and inform future policy recommendations aimed at improving prevention, treatment and recovery outcomes across Europe.
“Improving schizophrenia care requires coordinated action across research, health systems and policy.”